Important Information about Diverticula, Diverticulosis and Diverticulitis
May 2, 2026 Jane Jackson, RN, CRC BHealthyRN
Diverticulosis and diverticulitis have similar names and are related, yet they are distinctly different diagnoses. The similarity in their names could be highly confusing.
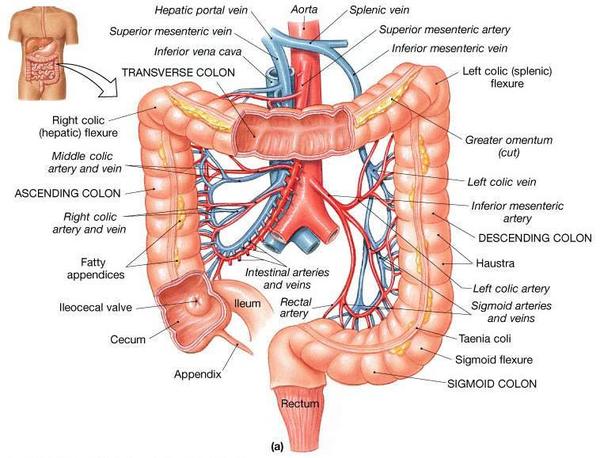
Diverticulosis is the formation of abnormal pockets called diverticula in the lining of the lower large intestine – especially in the sigmoid colon. A low-fiber diet often causes this. It becomes hard and difficult to pass without sufficient fiber to soften fecal matter.
The increased pressure required to force the hardened stool through the colon causes small pockets to form at weak points in the wall of the colon – especially in the sigmoid colon. Nearly 50% of people over 65 have developed diverticulosis.
Unfortunately, once diverticulosis forms, it will not resolve. The good news is that it does not usually cause symptoms and may only be detected during routine imaging.
Diverticulitis occurs when diverticula from the diverticulosis become inflamed and/or infected. The inflamed diverticula causes sudden, severe abdominal pain that often intensifies over several days. Fever, chills, nausea, vomiting, constipation, or diarrhea can accompany this pain. Nearly 3500 people die from diverticulitis every year.
Other common symptoms of diverticulitis are cramping and bloating accompanied by the constant urge for fecal elimination. There may be blood in the stool. A more serious complication is the rupture of an inflamed diverticulum, which releases intestinal content into the abdomen, resulting in peritonitis – an inflammation of the abdominal cavity’s lining. Peritonitis is a potentially life-threatening condition. It can be treated with IV antibiotics usually in a hospital setting. Antibiotics will fight the infection but sometimes, peritonitis requires surgery to repair the rupture or to remove a portion of the damaged area of the large intestine.
Stress and smoking make symptoms worse. Even a family history of gallbladder disease, obesity and/or coronary artery disease can increase the potential for developing diverticulosis and the potential of diverticulitis. There is no way to predict if diverticulosis will develop into diverticulitis. Nearly 1 in 4 who develop diverticulitis, will have one or more of the following complications
- An abscess – an infected pouch that becomes swollen and filled with pus
- A fistula – an abnormal passageway between the bowel and other organs
- Intestinal obstruction – a blockage preventing stool the passage of stool
- A perforation/rupture – a hole in the colon
- Peritonitis – an infection in the abdominal cavity
Asymptomatic diverticulosis does not require treatment. Patients are often advised to increase dietary fiber and stay well‑hydrated. Some individuals use fiber supplements such as methylcellulose or psyllium to help support regularity.
Diverticulitis requires medical treatment. Patients with mild symptoms usually are prescribed IV antibiotics and may be placed on a liquid diet until the diverticulitis resolves. In the presence of diverticular bleeding, immediate medical attention is required. Procedures such as a colonoscopy or surgery may be necessary.
Some lifestyle strategies to avoid diverticulosis and diverticulitis are
- Maintaining a normal BMI
- Smoking cessation
- Consuming a high-fiber diet
- Exercising regularly
- Limit NSAID use (Avoid taking ibuprofen and aspirin. NOTE: If you take aspirin for cardiovascular disease – talk with your healthcare professional before discontinuing a prescribed medication.)
Once diagnosed with diverticulosis, it is important to maintain a regular bowel pattern to prevent progression to diverticulitis. Mild diverticulitis can be treated with bed rest, stool softeners, a liquid diet, antibiotics to fight the infection, and possibly antispasmodic drugs. Seek healthcare professional treatment to avoid potential life-threatening complications. After multiple bouts with inflammatory diverticulitis, surgery may be recommended to remove the affected section of the large intestine. Full recovery is probable if you receive prompt medical attention.
To potentially the Diverticula – Diverticulosis – Diverticulitis cycle – some people use fiber supplements or stool softeners as part of their daily routine. Consume at least 30 grams of fiber and ten – 8 oz glasses of water, tea, broth, or juice daily. Fiber supplements or stool softeners can be added daily to help maintain a regular bowel elimination pattern. Stool softeners that contain methylcellulose or psyllium do not promote gas formation in the colon. Some laxatives may irritate the bowel; a healthcare professional can help determine what’s appropriate.
This information has not been approved by the Food and Drug Administration. These products are not approved to cure, treat, or prevent a disease. Consult a healthcare professional before starting a dietary supplement, especially if you have medical conditions or prescribed medications. This article is for educational purposes and not to replace the advice of your healthcare professional.


